Connect With Us
vendor
What Is Sever’s Disease?
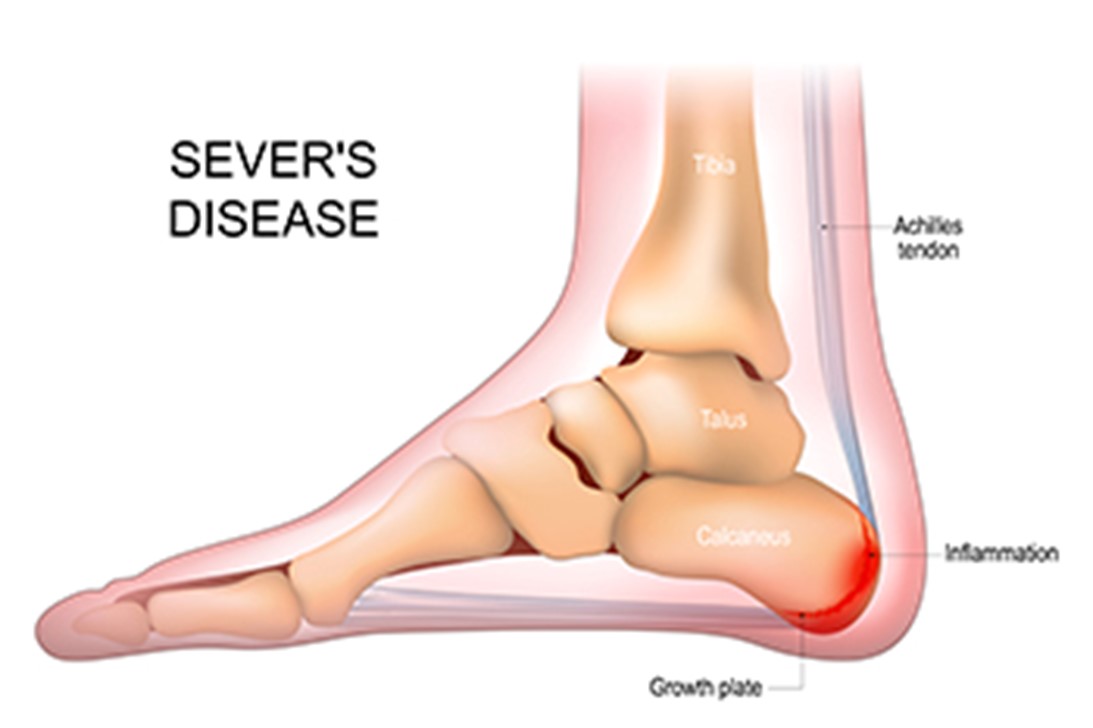 Sever’s disease is a frequent cause of heel pain in children going through their growth spurt, typically between the ages of eight and 14. This condition arises when the Achilles tendon, which links the calf muscle to the heel, grows slower than the bones in the feet. As a result, the tendon pulls on the heel, causing discomfort. Symptoms can include heel pain during or after physical activity, limping, and walking on tiptoes. Though Sever’s disease often improves as growth slows, there are effective methods that can manage the pain. Adjusting activity levels, taking medications, and using orthotics can provide relief. If your child is struggling with heel pain, it is suggested you schedule an appointment with a podiatrist who can offer a proper diagnosis and recommend the best course of action to ensure your child’s comfort and continued activity.
Sever’s disease is a frequent cause of heel pain in children going through their growth spurt, typically between the ages of eight and 14. This condition arises when the Achilles tendon, which links the calf muscle to the heel, grows slower than the bones in the feet. As a result, the tendon pulls on the heel, causing discomfort. Symptoms can include heel pain during or after physical activity, limping, and walking on tiptoes. Though Sever’s disease often improves as growth slows, there are effective methods that can manage the pain. Adjusting activity levels, taking medications, and using orthotics can provide relief. If your child is struggling with heel pain, it is suggested you schedule an appointment with a podiatrist who can offer a proper diagnosis and recommend the best course of action to ensure your child’s comfort and continued activity.
Sever's disease often occurs in children and teens. If your child is experiencing foot or ankle pain, see one of our clinicians from The Footcare Centre. Our podiatrists can treat your child’s foot and ankle needs.
Sever’s Disease
Sever’s disease is also known as calcaneal apophysitis, which is a medical condition that causes heel pain in none or both feet. The disease is known to affect children between the ages of 8 and 14.
Sever’s disease occurs when part of the child’s heel known as the growth plate (calcaneal epiphysis) is attached to the Achilles tendon. This area can suffer injury when the muscles and tendons of the growing foot do not keep pace with bone growth. Therefore, the constant pain that one experiences at the back of the heel will make the child unable to put any weight on the heel. The child is then forced to walk on their toes.
Symptoms
Acute pain – Pain associated with Sever’s disease is usually felt in the heel when the child engages in physical activity such as walking, jumping, and or running.
Highly active – Children who are very active are among the most susceptible in experiencing Sever’s disease, because of the stress and tension placed on their feet.
If you have any questions please feel free to contact our offices located in Weybridge, UK. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Sever's Disease
Sever’s disease, also known as calcaneal apophysitis is a common bone disorder that occurs during childhood. The disease is defined as an inflammation of the growth plate in the heel. When a child has a growth spurt, his heel bone grows faster than the muscles, tendons, and ligaments in his leg. This disease is a result of overuse. The people who are most likely to be affected by this disease are children who are in a growth spurt, especially boys who are from the ages of 5 to 13 years old. 60% of children with Sever’s disease have both heels involved.
Symptoms of this disease are heel pain that intensifies during running and jumping activities. The pain is typically localized to the posterior part of the heel. Symptoms may be severe, and they can easily interfere with daily activities. Children who play soccer, baseball, and basketball are more likely to develop Sever’s disease.
Your podiatrist will diagnose your child based on his or her symptoms, x-rays are generally not helpful in diagnosing this disease. Your podiatrist may examine both heels and ask your child questions about his or her activity level in sports. Your podiatrist may then use the squeeze test on your child’s heel to see if there is any pain. Nevertheless, some podiatrists might still use x-rays to rule out any other issues such as fractures, infections, and tumors.
Sever’s disease can be prevented by maintaining good flexibility while your child is growing. Another prevention method is to wear good-quality shoes that have firm support and a shock-absorbent sole. Sever’s disease can be treated by ceasing any activity that causes heel pain. You should apply ice to the injured heel for 20 minutes 3 times a day. Additionally, orthotics should be used for children who have high arches, flat feet, or bowed legs.
If you suspect your child has Sever’s disease, you should make an appointment with your podiatrist to have his or her foot examined. Your podiatrist may recommend nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen to relieve pain. In more severe cases, your child may need a cast to rest his or her heel. Fortunately, Sever’s disease does not cause long-term foot problems. After treatment, your child should start to feel better within two weeks to two months.
All About Ankle Pain
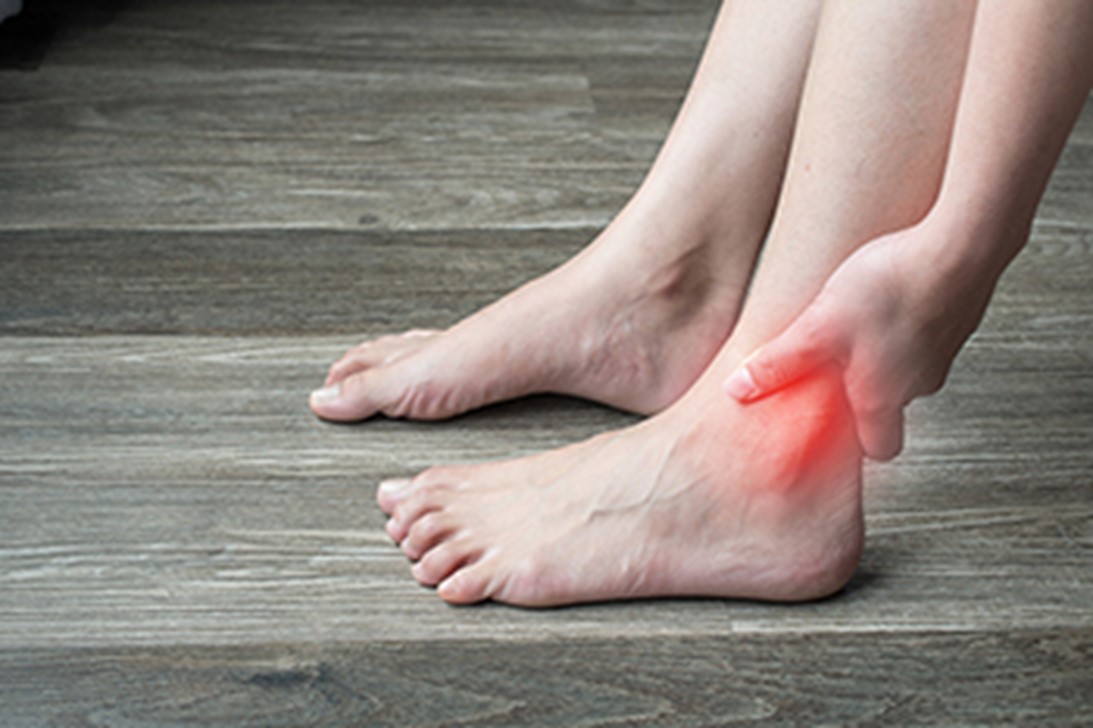 Ankle pain can stem from various issues affecting the complex structure of the ankle, which includes bones, ligaments, tendons, and muscles. The ankle joint comprises the tibia and fibula bones of the lower leg, which connect to the talus bone in the foot. Ligaments stabilize the joint, while tendons enable movement. Common causes of ankle pain can include sprains, arthritis, and fractures. Sprains occur when ligaments are stretched or torn, often due to twisting injuries. Strains involve overstretching or tearing of tendons or muscles. Arthritis can lead to inflammation and stiffness, while fractures result from trauma or severe impact. To alleviate ankle pain, consider resting the ankle to reduce swelling and discomfort. Mild pain relievers like ibuprofen may also help to provide temporary relief. For persistent or severe pain, it is suggested you contact a podiatrist for professional medical advice, as more advanced treatments may be necessary to address the underlying issue and restore function.
Ankle pain can stem from various issues affecting the complex structure of the ankle, which includes bones, ligaments, tendons, and muscles. The ankle joint comprises the tibia and fibula bones of the lower leg, which connect to the talus bone in the foot. Ligaments stabilize the joint, while tendons enable movement. Common causes of ankle pain can include sprains, arthritis, and fractures. Sprains occur when ligaments are stretched or torn, often due to twisting injuries. Strains involve overstretching or tearing of tendons or muscles. Arthritis can lead to inflammation and stiffness, while fractures result from trauma or severe impact. To alleviate ankle pain, consider resting the ankle to reduce swelling and discomfort. Mild pain relievers like ibuprofen may also help to provide temporary relief. For persistent or severe pain, it is suggested you contact a podiatrist for professional medical advice, as more advanced treatments may be necessary to address the underlying issue and restore function.
Ankle Pain
Ankle pain can be caused by a number of problems and may be potentially serious. If you have ankle pain, consult with one of our clinicians from The Footcare Centre. Our podiatrists will assess your condition and provide you with quality foot and ankle treatment.
Ankle pain is any condition that causes pain in the ankle. Due to the fact that the ankle consists of tendons, muscles, bones, and ligaments, ankle pain can come from a number of different conditions.
Causes
The most common causes of ankle pain include:
- Types of arthritis (rheumatoid, osteoarthritis, and gout)
- Ankle sprains
- Broken ankles
- Achilles tendonitis
- Achilles tendon rupture
- Stress fractures
- Bursitis
- Tarsal tunnel syndrome
- Plantar fasciitis
Symptoms
Symptoms of ankle injury vary based upon the condition. Pain may include general pain and discomfort, swelling, aching, redness, bruising, burning or stabbing sensations, and/or loss of sensation.
Diagnosis
Due to the wide variety of potential causes of ankle pain, podiatrists will utilize a number of different methods to properly diagnose ankle pain. This can include asking for personal and family medical histories and of any recent injuries. Further diagnosis may include sensation tests, a physical examination, and potentially x-rays or other imaging tests.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are rest, ice packs, keeping pressure off the foot, orthotics and braces, medication for inflammation and pain, and surgery.
If you have any questions please feel free to contact our offices located in Weybridge, UK. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Ankle Pain
The ankle joint is the point at which the bones of the leg and foot join. This joint is crucial because it is responsible for the foot’s mobility. Ankle pain is typically the result of inflammation from an injury to bones, joint space, cartilage, ligaments, tendons, or muscles in the area. Commonly associated symptoms with ankle pain are bruising, redness, numbness, stiffness, weakness, and tingling.
The most common causes of ankle pain are sprains and injuries. Ankle sprains are one of the most common musculoskeletal injuries. Sprains occur when the ligaments of the ankle become partially or completely torn due to sudden stretching. Sprains can occur on either the inner or outer sides of the ankle joint. Usually, these injuries occur when the ankle is twisted in an activity by stepping off an uneven surface. More specific causes include rheumatoid arthritis, gout, osteoarthritis, and Achilles tendonitis.
If you are experiencing ankle pain, you should consult with your podiatrist to choose the best method of care. Your doctor will conduct an examination of your ankle to determine the underlying cause of the pain.
Selecting the Right Shoes for Children
 Children are typically born with flat feet, a natural condition due to undeveloped arches and soft, flexible bones. As they grow, their arches gradually form, usually becoming noticeable around age two or three. During the early years, it is best for children to walk barefoot as much as possible, allowing their feet to develop strength and proper alignment. When they begin walking outdoors, they need shoes that provide protection without restricting natural foot movement. Look for shoes with a flexible sole, breathable material, and a wide toe box to accommodate growing feet. Shoes should also have a snug fit at the heel to prevent slipping but not be too tight to cause discomfort. Regularly checking for proper fit is important, as children’s feet grow rapidly. When it comes time to select shoes for your child, it is suggested that you schedule an appointment with a podiatrist for further help and to have your child’s feet assessed for any other footwear needs for healthy foot development.
Children are typically born with flat feet, a natural condition due to undeveloped arches and soft, flexible bones. As they grow, their arches gradually form, usually becoming noticeable around age two or three. During the early years, it is best for children to walk barefoot as much as possible, allowing their feet to develop strength and proper alignment. When they begin walking outdoors, they need shoes that provide protection without restricting natural foot movement. Look for shoes with a flexible sole, breathable material, and a wide toe box to accommodate growing feet. Shoes should also have a snug fit at the heel to prevent slipping but not be too tight to cause discomfort. Regularly checking for proper fit is important, as children’s feet grow rapidly. When it comes time to select shoes for your child, it is suggested that you schedule an appointment with a podiatrist for further help and to have your child’s feet assessed for any other footwear needs for healthy foot development.
Making sure that your children maintain good foot health is very important as they grow. If you have any questions, contact one of our clinicians from The Footcare Centre. Our podiatrists can provide the care you need to keep you pain-free and on your feet.
Keeping Children's Feet Healthy
Having healthy feet during childhood can help prevent medical problems later in life, namely in the back and legs. As children grow, their feet require different types of care. Here are some things to consider...
Although babies do not walk yet, it is still very important to take care of their feet.
Avoid putting tight shoes or socks on his or her feet.
Allow the baby to stretch and kick his or her feet to feel comfortable.
As a toddler, kids are now on the move and begin to develop differently. At this age, toddlers are getting a feel for walking, so don’t be alarmed if your toddler is unsteady or ‘walks funny’.
As your child gets older, it is important to teach them how to take care of their feet.
Show them proper hygiene to prevent infections such as fungus.
Be watchful for any pain or injury.
Have all injuries checked by a doctor as soon as possible.
Comfortable, protective shoes should always be worn, especially at play.
If you have any questions please feel free to contact our offices located in Weybridge, UK. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
How to Care for Your Child's Feet
It is never normal for a child to experience pain in his or her feet. Foot pain that lasts more than a few days and limits a child’s ability to walk should be examined by a podiatrist. Many adult foot ailments originate in childhood and may be present at birth. Common foot issues that are experienced by children are pediatric flat foot, Sever’s disease, ingrown toenails, and plantar warts.
A child’s foot grows rapidly during the first year, allowing it to reach almost half of their adult foot size. Consequently, foot specialists consider the first year to be the most crucial point in the foot development process. There are ways you can help ensure that your child’s foot develops properly. One way is to carefully look at your baby’s feet. If you notice any deformities, you should immediately seek professional care. You should also loosely cover your child’s foot, since tight coverings may prevent movement and inhibit normal development. Another tip is to change the baby’s positioning throughout the day. If your baby lies down in one spot for too long, it may put an excess amount of strain on the feet and legs.
It is best that you try not to force a child to start walking. Children will begin to walk when they are both physically and emotionally capable to do so. You should also avoid comparing your child’s walking progress with other children because the age range for independent walking may range. When your child’s feet begin to develop, you may need to change both their shoe and sock size every few months to allow room for their feet to grow.
Kids are sometimes prone to splinters, cuts, and severe injuries because they tend to walk around barefoot. This also makes them more susceptible to developing plantar warts which is a condition caused by a virus that invades the sole of the foot through breaks in the skin. These ailments can be avoided by making sure your child wears shoes in unsanitary environments. You should also wash any minor cuts or scrapes on your child’s feet. It is a myth that exposure to fresh air will heal injuries; fresh air will only expose your child’s cuts to germs.
As a parent, you should ensure that your child’s feet are developing properly and are being properly maintained. Consequently, it is important that you perform routine inspections on his or her feet to detect any injuries or deformities in their early stages. Early detection and treatment will help to ensure that your child does not develop any serious foot conditions.
Treatment for Hammertoes
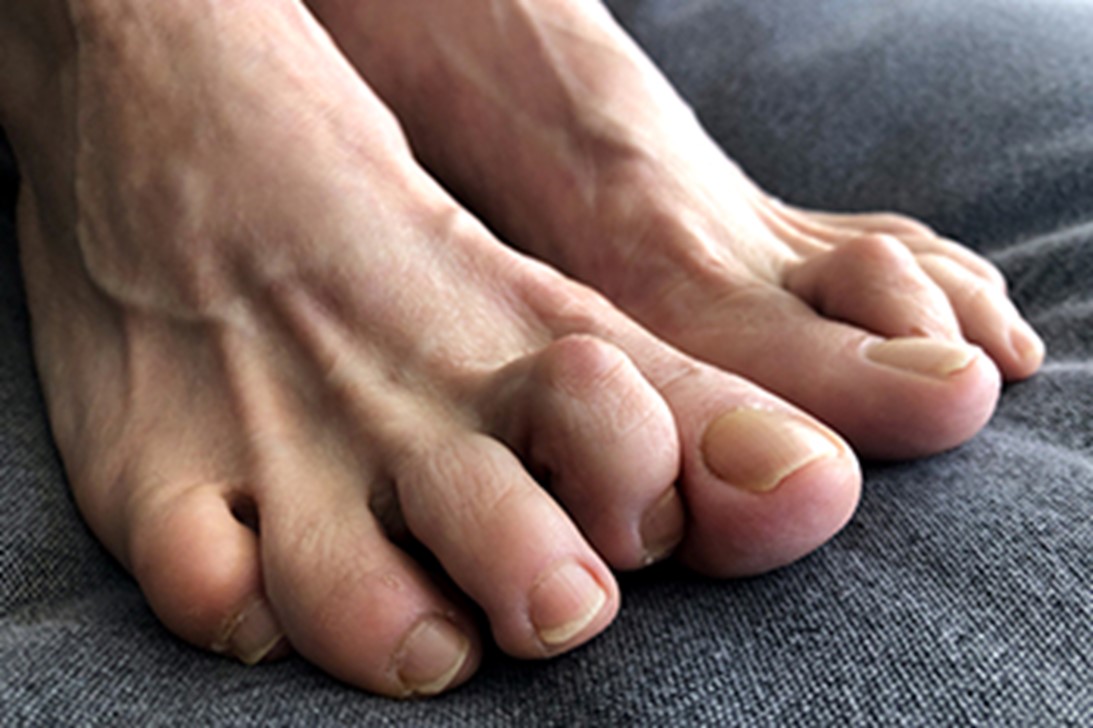 Hammertoes, also known as claw toes or mallet toes, are deformities where one or more toes bend abnormally at the middle joint, resembling a hammer. This condition can range from mild to severe. In mild cases, toes may still be flexible and only slightly bent, causing minimal discomfort. Severe cases can involve rigid, painful toes that can lead to corns, calluses, and difficulty in walking. Hammertoes often result from wearing tight, narrow shoes that force the toes into a bent position. They can also be caused by muscle imbalances, arthritis, or genetic predisposition. Treatments vary based on severity. Mild cases can benefit from switching to roomier footwear, using orthotic devices, wearing splints, and performing toe exercises. Severe cases may require medical interventions such as corticosteroid injections or surgical correction. If you have severe pain from a hammertoe, it is suggested that you consult a podiatrist for the best ways to relieve discomfort and restore toe function.
Hammertoes, also known as claw toes or mallet toes, are deformities where one or more toes bend abnormally at the middle joint, resembling a hammer. This condition can range from mild to severe. In mild cases, toes may still be flexible and only slightly bent, causing minimal discomfort. Severe cases can involve rigid, painful toes that can lead to corns, calluses, and difficulty in walking. Hammertoes often result from wearing tight, narrow shoes that force the toes into a bent position. They can also be caused by muscle imbalances, arthritis, or genetic predisposition. Treatments vary based on severity. Mild cases can benefit from switching to roomier footwear, using orthotic devices, wearing splints, and performing toe exercises. Severe cases may require medical interventions such as corticosteroid injections or surgical correction. If you have severe pain from a hammertoe, it is suggested that you consult a podiatrist for the best ways to relieve discomfort and restore toe function.
Hammertoe
Hammertoes can be a painful condition to live with. For more information, contact one of our clinicians from The Footcare Centre. Our podiatrists will answer any of your foot- and ankle-related questions.
Hammertoe is a foot deformity that affects the joints of the second, third, fourth, or fifth toes of your feet. It is a painful foot condition in which these toes curl and arch up, which can often lead to pain when wearing footwear.
Symptoms
- Pain in the affected toes
- Development of corns or calluses due to friction
- Inflammation
- Redness
- Contracture of the toes
Causes
Genetics – People who are genetically predisposed to hammertoe are often more susceptible
Arthritis – Because arthritis affects the joints in your toes, further deformities stemming from arthritis can occur
Trauma – Direct trauma to the toes could potentially lead to hammertoe
Ill-fitting shoes – Undue pressure on the front of the toes from ill-fitting shoes can potentially lead to the development of hammertoe
Treatment
Orthotics – Custom made inserts can be used to help relieve pressure placed on the toes and therefore relieve some of the pain associated with it
Medications – Oral medications such as anti-inflammatories or NSAIDs could be used to treat the pain and inflammation hammertoes causes. Injections of corticosteroids are also sometimes used
Surgery – In more severe cases where the hammertoes have become more rigid, foot surgery is a potential option
If you have any questions please feel free to contact our offices located in Weybridge, UK. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Hammertoe
Hammertoe is a foot deformity that occurs due to an imbalance in the tendons, muscles, or ligaments that are responsible for holding the toes in their normal position. This condition may be caused by poor footwear, foot structure, trauma, and disease. The most common solution for hammertoe is to relieve the pain by changing your footwear and wearing orthotics. In severe cases, surgery may be required.
The shoes that are most likely to cause hammertoe are high heeled shoes or shoes that are too tight in the toe box. Tight shoes will force your toes to crowd together in a curled position. This position will likely continue when you take your shoes off. Another cause is trauma. When you stub your toe, you are increasing the chance that you will develop hammertoe.
There are risk factors that may make you more likely to develop this condition. Women are more likely to have the condition compared to men, and it is also more likely to appear in those who are older in age.
Many different foot problems can be avoided by wearing shoes that have adjustability, adequate toe room, and low heels. Furthermore, if you want to buy new shoes, you should look to purchase them at the end of the day and make sure you know your correct size. The importance of buying shoes at the end of the day is that your feet swell as the day progresses. You should also ensure that you are wearing your correct size because your shoe size may change as you grow older.
To diagnose someone with hammertoe, your podiatrist will need to conduct a thorough examination of your foot. Your doctor may even order an x-ray to evaluate the bones and joints of your feet and toes.
If you have hammertoe, your podiatrist may recommend that you wear shoes that fit you better along with inserts to place inside them. Additionally, he or she may suggest special exercises for you to perform to stretch your toes. One helpful exercise it to pick up marbles with your feet or crumple a towel with your toes.
Prior to meeting with your podiatrist, it will be helpful to make a list of all the symptoms you are experiencing. You should also make a note of medications you are taking and important personal information about your medical history.
Foot Conditions During Pregnancy
 Pregnancy can bring forth several foot conditions that impact comfort and mobility. As weight naturally increases, the arch of the foot may flatten, leading to overpronation and strain on the plantar fascia, potentially causing plantar fasciitis. This condition causes pain along the bottom of the foot, particularly near the heel, worsened by standing or walking for extended periods. Hormonal changes during pregnancy contribute to ligament laxity, further destabilizing the foot's structure and increasing the risk of injuries. To alleviate discomfort, wearing supportive footwear with cushioning and arch support is essential. Regular stretching exercises targeting the calves and plantar fascia help maintain flexibility and reduce tension. Managing weight gain through appropriate exercise and a balanced diet can also ease the strain on the feet. If you have persistent foot pain during your pregnancy, it is suggested that you consult a podiatrist who can offer you effective relief options.
Pregnancy can bring forth several foot conditions that impact comfort and mobility. As weight naturally increases, the arch of the foot may flatten, leading to overpronation and strain on the plantar fascia, potentially causing plantar fasciitis. This condition causes pain along the bottom of the foot, particularly near the heel, worsened by standing or walking for extended periods. Hormonal changes during pregnancy contribute to ligament laxity, further destabilizing the foot's structure and increasing the risk of injuries. To alleviate discomfort, wearing supportive footwear with cushioning and arch support is essential. Regular stretching exercises targeting the calves and plantar fascia help maintain flexibility and reduce tension. Managing weight gain through appropriate exercise and a balanced diet can also ease the strain on the feet. If you have persistent foot pain during your pregnancy, it is suggested that you consult a podiatrist who can offer you effective relief options.
Pregnant women with swollen feet can be treated with a variety of different methods that are readily available. For more information about other cures for swollen feet during pregnancy, consult with one of our clinicians from The Footcare Centre. Our podiatrists will attend to all of your foot and ankle needs.
What Foot Problems Can Arise During Pregnancy?
One problem that can occur is overpronation, which occurs when the arch of the foot flattens and tends to roll inward. This can cause pain and discomfort in your heels while you’re walking or even just standing up, trying to support your baby.
Another problem is edema, or swelling in the extremities. This often affects the feet during pregnancy but tends to occur in the later stages.
How Can I Keep My Feet Healthy During Pregnancy?
- Wearing orthotics can provide extra support for the feet and help distribute weight evenly
- Minimize the amount of time spent walking barefoot
- Wear shoes with good arch support
- Wear shoes that allow for good circulation to the feet
- Elevate feet if you experience swelling
- Massage your feet
- Get regular, light exercise, such as walking, to promote blood circulation to the feet
If you have any questions please feel free to contact our offices located in Weybridge, UK. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Pregnancy and Foot Health
Many pregnant women complain about foot pain while they are expecting. Foot pain can primarily be caused by weight gain and hormonal changes taking place in the body. By understanding how pregnancy impacts the health of a woman's feet, a pregnant woman can take action to keep her feet as healthy and comfortable as possible.
Because a woman's weight changes during pregnancy, more pressure is brought to bear on both the legs and the feet. This weight shift can cause two major foot problems: over-pronation, also known as flat feet, as well as edema, which is swelling of the feet. Over-pronation occurs when the arch of the foot flattens, causing the foot to roll inwards when the individual is walking, and can aggravate the plantar fascia tissues located along the bottom of the feet. If these tissues become inflamed, a pregnant woman can experience pain in the heel of the foot as well as severe foot pain while walking or standing. Swelling of the feet, or edema, often occurs in the later stages of pregnancy. It is caused by slow circulation and water retention, and may turn the feet a light purple color.
To keep feet in good health and prevent over-pronation, pregnant women should avoid walking barefoot and be sure they are wearing shoes that offer good arch support. A device known as an orthotic can be added to regular footwear in order to provide additional support for the feet during pregnancy. Any expectant mother whose feet hurt should first check to see if the shoes she is wearing are old, worn out and not offering the proper support necessary for distributing the weight of her body during pregnancy.
To treat edema of the feet, a good start is to wear quality footwear which offers support and good circulation. Keep feet elevated whenever possible by using a foot stool while seated. Stay well hydrated by drinking plenty of water to prevent water retention in the feet. Any swelling that occurs in only one foot should be examined as soon as possible by a podiatrist.
Good foot health during pregnancy can help expectant mothers avoid foot pain that leads to other health problems. Massaging the feet and doing regular gentle exercise like walking aids foot health by contributing to good circulation. Supportive shoes are also a good investment that will support foot health during pregnancy.
