Connect With Us
Blog
Foot Arthritis and Finding Relief
 Foot arthritis encompasses several conditions that can cause pain and inflammation in the joints. Rheumatoid arthritis is an autoimmune disorder that leads to chronic inflammation, often affecting multiple joints in the feet. Psoriatic arthritis, associated with psoriasis, can also impact the toes and joints, causing swelling and discomfort. Osteoarthritis, a degenerative joint disease, results from wear and tear over time, leading to stiffness and pain. Gout, characterized by sudden and severe pain, occurs when uric acid crystals accumulate in the joints, frequently affecting the big toe. Finding relief from foot arthritis involves a combination of strategies. Resting and elevating the feet can help reduce swelling. Wearing supportive footwear and engaging in low-impact exercises can improve mobility and enhance overall foot health. If you have arthritic foot symptoms, it is suggested that you consult a podiatrist who can offer you effective relief options.
Foot arthritis encompasses several conditions that can cause pain and inflammation in the joints. Rheumatoid arthritis is an autoimmune disorder that leads to chronic inflammation, often affecting multiple joints in the feet. Psoriatic arthritis, associated with psoriasis, can also impact the toes and joints, causing swelling and discomfort. Osteoarthritis, a degenerative joint disease, results from wear and tear over time, leading to stiffness and pain. Gout, characterized by sudden and severe pain, occurs when uric acid crystals accumulate in the joints, frequently affecting the big toe. Finding relief from foot arthritis involves a combination of strategies. Resting and elevating the feet can help reduce swelling. Wearing supportive footwear and engaging in low-impact exercises can improve mobility and enhance overall foot health. If you have arthritic foot symptoms, it is suggested that you consult a podiatrist who can offer you effective relief options.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact one of our clinicians from The Footcare Centre. Our podiatrists can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a joint disorder that involves the inflammation of different joints in your body, such as those in your feet. Arthritis is often caused by a degenerative joint disease and causes mild to severe pain in all affected areas. In addition to this, swelling and stiffness in the affected joints can also be a common symptom of arthritis.
In many cases, wearing ill-fitting shoes can worsen the effects and pain of arthritis. Wearing shoes that have a lower heel and extra room can help your feet feel more comfortable. In cases of rheumatoid arthritis, the arch in your foot may become problematic. Buying shoes with proper arch support that contour to your feet can help immensely.
Alleviating Arthritic Pain
- Exercises that stretch the foot can prevent further pain and injury and increase mobility
- Most of the pain can be alleviated with anti-inflammatory drugs, heat, and topical medications
- Massages can help temporarily alleviate pain.
It is best to see your podiatrist for the treatment that is right for your needs and symptoms. Conditions vary, and a podiatrist can help you determine the right method of care for your feet.
If you have any questions please feel free to contact our offices located in Weybridge, UK. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Arthritic Foot Care
During your lifetime, you will probably walk about 75,000 miles, which is quite a lot of stress to put on your feet. As you get older, the 26 bones and 30 joints in each of your feet will lose flexibility and elasticity. Your foot’s natural shock absorbers will wear down as well. Having arthritis added to this mix only makes matters worse. Your joints will become distorted and inflamed, which is why arthritic foot care needs to be something to think about every day.
When dealing with arthritis, having additional foot complications, such as bunions, hammertoes, or neuroma, can be a serious detriment. To avoid these, buy well-fitting shoes with a lower heel and good support. Arthritis causes you to lose your arch, so having shoes with good arch support is also highly recommended.
Aside from getting good arch support, the shoes need to fit comfortably and properly as well. A good place to start is by leaving a finger width between the back of the shoe and your foot to gauge proper size. It is also helpful to have a square or rounded toe box in the front to provide even more comfort. Another thing to look for is a rubber sole that can provide a cushion and absorb shock as you walk. This adds flexibility to the ball of your foot when you push off your heel to walk.
Exercise is another key aspect of arthritic foot care. Exercise not only strengthens and stretches your muscles and joints, but helps to prevent further injury and pain as well. Stretching the Achilles tendon, the tendon located in the back of your heel, will give you added mobility and reduce pain due to stress. Another thing you can do is massage your feet, kneading the ball of your foot as well as your toes from top to bottom.
Stretching the Achilles tendon is a simple exercise that you can do at home anytime. Lean against the wall with your palms flat against the surface while placing one foot forward, towards the wall, and one foot behind you. Bend your forward knee towards the wall while keeping your back knee locked straight, and make sure both your heels are completely touching the ground at all times. This will stretch your Achilles tendon and calf muscles as well. You will feel the stretch almost immediately. You can also stretch your toes in a couple ways. One involves taking a rubber band and wrapping it around both your big toes while your heels remain together. Then, pull them apart to stretch your big toe. You can also place a rubber band around all the toes of one of your feet. Then, try to separate each individual toe, stretching them all.
A final step you can take to help your arthritis is taking non-steroid, non-inflammatory drugs or topical medicines with capsaicin. Unfortunately, there is no complete way to remove all of your arthritic pain. However, following some of this advice can go a long way in staying as pain-free as possible.
Running Blisters and How to Prevent Them
 A running blister is a painful pocket of fluid that forms between layers of skin due to friction. This common injury occurs when repetitive rubbing from shoes or socks irritates the skin, causing it to separate and fill with fluid. Blisters are most likely to appear on the feet, particularly on the heels, toes, or soles, during long runs or intense physical activity. Prevention is key to avoiding blisters. Wearing well-fitted shoes that provide proper support and minimize friction is essential. Choosing moisture-wicking socks can help reduce the build-up of sweat, which increases the risk of blister formation. Using blister prevention tape or cushioned insoles can provide additional protection in high-risk areas. Finally, gradually increasing running distances allows the feet to adapt, reducing the likelihood of blisters. Foot blisters can be uncomfortable and may become infected if not properly treated. If you have a foot blister, it is suggested that you contact a podiatrist for proper treatment and prevention techniques.
A running blister is a painful pocket of fluid that forms between layers of skin due to friction. This common injury occurs when repetitive rubbing from shoes or socks irritates the skin, causing it to separate and fill with fluid. Blisters are most likely to appear on the feet, particularly on the heels, toes, or soles, during long runs or intense physical activity. Prevention is key to avoiding blisters. Wearing well-fitted shoes that provide proper support and minimize friction is essential. Choosing moisture-wicking socks can help reduce the build-up of sweat, which increases the risk of blister formation. Using blister prevention tape or cushioned insoles can provide additional protection in high-risk areas. Finally, gradually increasing running distances allows the feet to adapt, reducing the likelihood of blisters. Foot blisters can be uncomfortable and may become infected if not properly treated. If you have a foot blister, it is suggested that you contact a podiatrist for proper treatment and prevention techniques.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact one of our clinicians from The Footcare Centre. Our podiatrists can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions please feel free to contact our offices located in Weybridge, UK. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Blisters
Blisters are small pockets of fluid that occur on the top layers of the skin for several reasons. Friction, burns, and diseases are all known causes of blisters. Smaller blisters are known as vesicles, while larger blisters are referred to as bulla. The fluid inside the bubble can be blood, pus, or serum; which is a clear liquid that protects the skin. In most cases, blisters are not a major health issue, but they can be an indicator of a more serious condition.
Causes of blisters vary. Blisters are commonly caused by wearing poorly fitted shoes that rub against the foot. However, there are many other causes besides from friction; including burns, sunburn, insect bites, frostbite, poison ivy/oak, chemical exposure, impetigo, eczema, viral infections, and more.
Most blisters heal by themselves and do not require immediate medical care. If you have a blister, do not pop it since this may cause infection; it is advised to put a bandage over the blister to protect it. If the blister is large, causes pain, or if you have a fever, it is recommended that you see a podiatrist who can provide proper care. Blisters are easy to diagnose, and if considered prudent by the podiatrist, can easily be drained of fluid with a sterile needle as well.
To prevent blisters on the feet, wear shoes that fit properly and don’t cause rubbing. Socks can help prevent friction and it is recommended that you wear them if you are wearing shoes. Hand blisters can be avoided by wearing gloves during activities that cause friction against the hand. If you have a blister that pops, do not remove the dead skin, wash the area, apply antibiotic ointment, and cover with a bandage. It is okay in most cases to not seek immediate medical care for a blister if it was just caused by friction. However, if the blister causes pain or does not go away, it is suggested that you see a podiatrist for a diagnosis.
What Causes Swollen Feet and Ankles?
 Swelling in the feet and ankles can be a sign of chronic venous insufficiency, or CVI, or heart failure, both of which affect circulation and fluid balance. CVI occurs when the veins in the legs cannot efficiently return blood to the heart, causing blood to pool, resulting in swelling, varicose veins, and pain. Heart failure, on the other hand, leads to fluid buildup throughout the body, including the feet, due to the heart's inability to pump blood effectively. Common symptoms of both conditions include swelling, heaviness, and discomfort in the feet and ankles, often worsened by prolonged standing or inactivity. Treatment for CVI may involve compression stockings, lifestyle changes, and medications, while heart failure may require managing underlying cardiovascular health. A podiatrist can play a critical role in managing foot symptoms associated with these conditions by recommending proper footwear, compression therapy, and providing guidance on exercises to improve circulation. If you experience persistent foot swelling, it is suggested that you schedule an appointment with a podiatrist for a thorough evaluation and personalized care plan.
Swelling in the feet and ankles can be a sign of chronic venous insufficiency, or CVI, or heart failure, both of which affect circulation and fluid balance. CVI occurs when the veins in the legs cannot efficiently return blood to the heart, causing blood to pool, resulting in swelling, varicose veins, and pain. Heart failure, on the other hand, leads to fluid buildup throughout the body, including the feet, due to the heart's inability to pump blood effectively. Common symptoms of both conditions include swelling, heaviness, and discomfort in the feet and ankles, often worsened by prolonged standing or inactivity. Treatment for CVI may involve compression stockings, lifestyle changes, and medications, while heart failure may require managing underlying cardiovascular health. A podiatrist can play a critical role in managing foot symptoms associated with these conditions by recommending proper footwear, compression therapy, and providing guidance on exercises to improve circulation. If you experience persistent foot swelling, it is suggested that you schedule an appointment with a podiatrist for a thorough evaluation and personalized care plan.
Swollen feet can be a sign of an underlying condition. If you have any concerns, contact one of our clinicians from The Footcare Centre. Our podiatrists can provide the care you need to keep you pain-free and on your feet.
Swollen feet are a common ailment among pregnant women and people who stand or sit for extended periods. Aging may increase the possibility of swollen feet and patients who are obese often notice when their feet are swelling too. There may be medical reasons why swollen feet occur:
- Phlebitis - A condition that causes the veins to become inflamed and can also cause leg pain.
- Liver disease - This may lead to low blood levels of albumin which is a protein. This can cause fluid in the blood to pass into the tissues and several areas of the body can become swollen.
- Heart failure - When the heart doesn’t pump properly the blood that is normally pumped back to the heart can pool in the veins of the legs causing swollen feet.
- Kidney disease - One of the main functions of the kidneys is releasing excess fluid in the body. This type of condition can make it difficult for the kidneys to function properly, and as a result the feet may become swollen.
- Deep-vein thrombosis (DVT)- This is a serious condition where blood clots form in the veins of the legs. They can block the return of blood from the legs to the heart which may cause the feet to swell. It is important to be treated by a podiatrist if this condition is present.
Swollen feet can also be caused by bone and tendon conditions, including fractures, arthritis, and tendinitis. Additionally, there may be skin and toenail conditions and an infection may cause the feet to swell. Patients who take medicine to treat high blood pressure may be prone to getting swollen feet.
Many patients elevate their feet to help relieve the swelling and this is generally a temporary remedy. When a podiatrist is consulted the reason behind the swelling can be uncovered and subsequently treated. If you have any questions please feel free to contact our offices located in Weybridge, UK. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
If you have any questions please feel free to contact our offices located in Weybridge, UK. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Swelling of the Feet
There are many reasons why patients experience swelling of the feet. It is rather common and may be a side effect of pregnancy or from sitting and standing for most of the day. Gravity could also play a role in the development of swollen feet. It is known that the weight of blood volume in our bodies is exerted on the veins in the legs and feet. The veins may not work as efficiently during the aging process, and this could make the blood flow backward causing swollen feet. Relief may be found when obese patients lose weight, and it may help to engage in compression therapy by wearing compression socks, stockings, or athletic sleeves. This method can release pressure on the feet and ankles which may help to reduce existing swelling. There are patients who have controlled their swollen feet by implementing healthy lifestyle changes. These can consist of reducing salt intake, incorporating a gentle exercise regime into the daily routine, and drinking plenty of fresh water. Swollen feet may be a temporary condition that affects people who travel via airplane or automobile, so it is beneficial to walk as frequently as possible even though it can be difficult. Swelling of the feet can also be indicative of other health issues so it is important to pay attention to any type of chest pain, mental confusion, dizziness, or fever. If you consistently have swollen feet, it is strongly suggested that you consult with a podiatrist who can help determine the cause and how to effectively treat it.
Heel Spurs are a Common Cause of Heel Pain
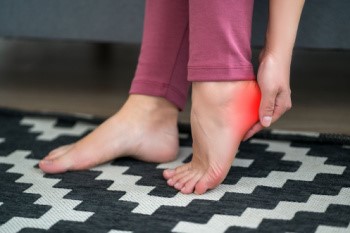 Heel spurs are a bony growth on the underside of the heel bone, often linked to heel pain and commonly associated with plantar fasciitis. While related, these are distinct conditions. Plantar fasciitis is inflammation of the tissue connecting the heel to the toes, while a heel spur is an actual calcium deposit on the heel. Heel spurs develop from repetitive stress, often due to excessive running, standing, or wearing improper footwear. Symptoms can include sharp pain, especially during initial steps in the morning, although some heel spurs are painless. To address heel spurs, treatments may involve rest and orthotic inserts to alleviate pressure and promote healing. Preventing heel spurs involves wearing supportive shoes, stretching, and avoiding prolonged impact. If you have persistent heel pain, it is suggested that you visit a podiatrist who can provide a tailored approach to management and advanced care for existing pain.
Heel spurs are a bony growth on the underside of the heel bone, often linked to heel pain and commonly associated with plantar fasciitis. While related, these are distinct conditions. Plantar fasciitis is inflammation of the tissue connecting the heel to the toes, while a heel spur is an actual calcium deposit on the heel. Heel spurs develop from repetitive stress, often due to excessive running, standing, or wearing improper footwear. Symptoms can include sharp pain, especially during initial steps in the morning, although some heel spurs are painless. To address heel spurs, treatments may involve rest and orthotic inserts to alleviate pressure and promote healing. Preventing heel spurs involves wearing supportive shoes, stretching, and avoiding prolonged impact. If you have persistent heel pain, it is suggested that you visit a podiatrist who can provide a tailored approach to management and advanced care for existing pain.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact one of our clinicians from The Footcare Centre. Our podiatrists will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main conditions spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions please feel free to contact our offices located in Weybridge, UK. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Heel Spurs
Heel spurs are the result of calcium deposits that cause bony protrusions on the underside of the heel. Heel spurs are usually painless, but they have the potential to cause heel pain. Heel spurs tend to be associated with plantar fasciitis, which is a condition that causes inflammation of the band of connective tissue that runs along the bottom of the foot. They most often occur to athletes whose sports involve a lot of running and jumping.
Some risk factors for developing heel spurs include running and jogging on hard surfaces, being obese, wearing poorly fitting shoes, or having walking gait abnormalities.
It is possible to have a heel spur without showing signs of any symptoms. However, if inflammation develops at the point of the spur’s formation, you may have pain while walking or running. In terms of diagnosis, sometimes all a podiatrist needs to know is that the patient is experiencing a sharp pain localized to the heel to diagnose a heel spur. Other times, an x-ray may be needed to confirm the presence of a heel spur.
Heel spurs can be prevented by wearing well-fitting shoes that have shock-absorbent soles. You should also be sure that you are choosing the right shoe for the activity you want to partake in; for example, do not wear walking shoes when you want to go on a run. Additionally, maintaining a healthy weight can be beneficial toward preventing heel spurs, as it will prevent an excess amount of pressure from being placed on the ligaments.
There are a variety of treatment options for people with heel spurs. Some of these include stretching exercises, physical therapy, shoe inserts, or taping and strapping to rest stressed muscles and tendons. If you have heel pain that lasts longer than a month, don’t hesitate to seek help from a podiatrist. Your podiatrist can help you determine which treatment option is best for you.
Causes and Relief Options for Toenail Fungus
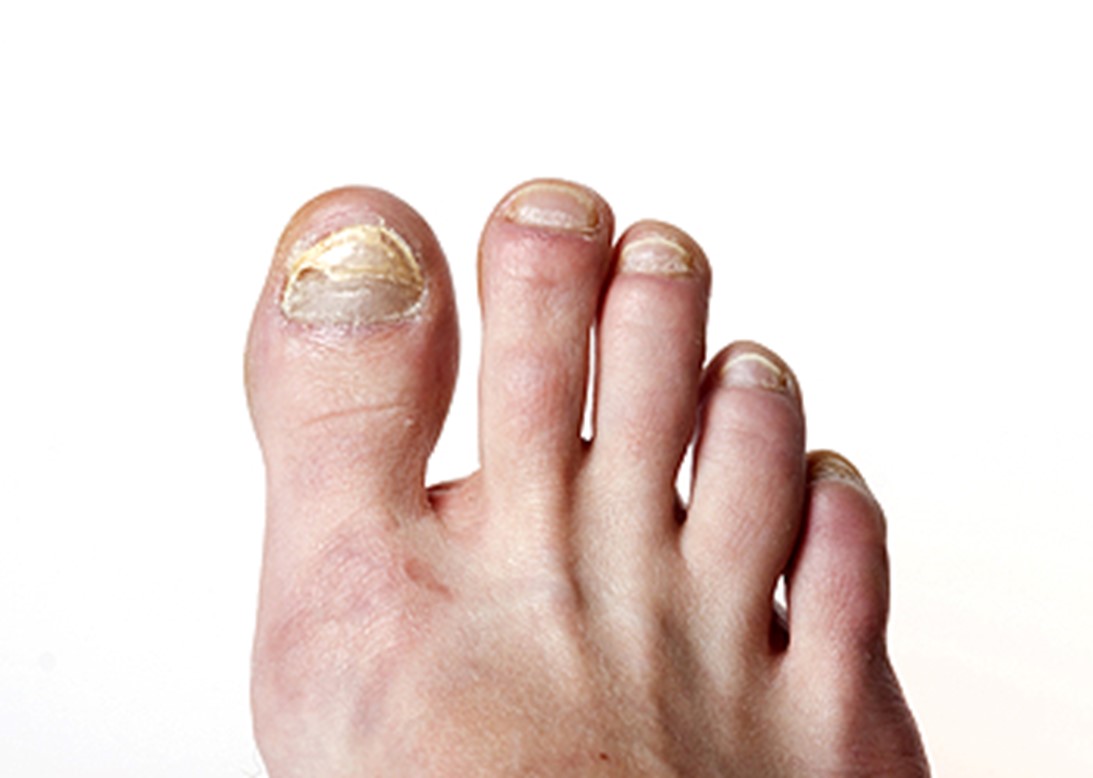 Toenail fungus, medically known as onychomycosis, is a common infection that affects the nail bed, often starting as a white or yellow spot under the nail. Over time, it can cause nails to thicken, discolor, crumble, or become misshapen, leading to discomfort, and, in some cases, pain. Toenail fungus thrives in warm, moist environments, making athletes, individuals who sweat heavily, and those who wear tight or non-breathable shoes more susceptible. Poor foot hygiene and minor nail injuries also increase risk. Treating toenail fungus can be challenging, as the infection tends to be persistent. For more stubborn infections, it is suggested that you schedule an appointment with a podiatrist who may prescribe oral antifungal medications or laser therapy to target the fungus.
Toenail fungus, medically known as onychomycosis, is a common infection that affects the nail bed, often starting as a white or yellow spot under the nail. Over time, it can cause nails to thicken, discolor, crumble, or become misshapen, leading to discomfort, and, in some cases, pain. Toenail fungus thrives in warm, moist environments, making athletes, individuals who sweat heavily, and those who wear tight or non-breathable shoes more susceptible. Poor foot hygiene and minor nail injuries also increase risk. Treating toenail fungus can be challenging, as the infection tends to be persistent. For more stubborn infections, it is suggested that you schedule an appointment with a podiatrist who may prescribe oral antifungal medications or laser therapy to target the fungus.
For more information about treatment, contact one of our clinicians from The Footcare Centre. Our podiatrists can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regimen for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open-toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture-wicking material also help as well.
If you have any questions please feel free to contact our offices located in Weybridge, UK. We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Toenail Fungus
Toenail fungus is a frustrating problem that affects many people. It can be persistent and hard to get rid of. As many different types of fungi are present throughout the environment, it is very easy to contract toenail fungus.
The feet are especially susceptible to toenail fungus because shoes and socks create the ideal dark and moist environment in which fungal infections thrive. While fungal infections of the nail plate are quite common, if left untreated they can spread beyond the toenail and into the skin and other parts of the body.
Signs of toenail fungus include a thickened nail that has become yellow or brown in color, a foul smell, and debris beneath the nail. The toe may become painful due to the pressure of a thicker nail or the buildup of debris.
Treatment for toenail fungus is most effective during the early stages of an infection. If there is an accumulation of debris beneath the nail plate, an ingrown nail or a more serious infection can occur. While each treatment varies between patients, your podiatrist may prescribe you oral medications, topical liquids, creams, or laser therapy. To determine the best treatment process for you, be sure to visit your podiatrist at the first signs of toenail fungus.
Blog Archives
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
